BE FOREWARNED: I use graphic images and gifs in this post that may actually induce a masturbation session. I recommend reading this article when you are free and won't be disturbed, or that you are sure you can resist the temptation to masturbate.
Ever heard of "No Fap November?"
Well if you hadn't, now you have.
Well if you hadn't, now you have.
"No Nut November" is a time when men abstain from masturbation for a number of reasons.
Some organizations like NoFap encourage abstinence from masturbation to "overcome porn addiction." Some people
believe that masturbation itself can be an addiction, and that No Nut
November is a good time to demonstrate to yourself that you are "master
of your domain."
It's been a while since my last post, so I'd like to take advantage of this year's No Fap November to talk about masturbation, how intact men masturbate, masturbation techniques to try, and masturbation techniques to avoid. I'd like to tell my personal story of how I discovered masturbation, how I developed bad masturbation habits, how they affected my sex life, and how I overcame them.
How do intact guys masturbate?
It's been a while since my last post, so I'd like to take advantage of this year's No Fap November to talk about masturbation, how intact men masturbate, masturbation techniques to try, and masturbation techniques to avoid. I'd like to tell my personal story of how I discovered masturbation, how I developed bad masturbation habits, how they affected my sex life, and how I overcame them.
How do intact guys masturbate?
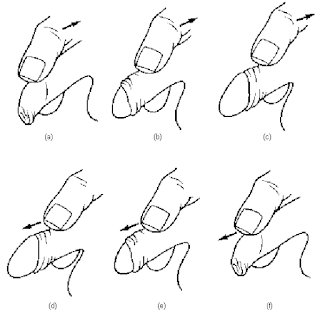
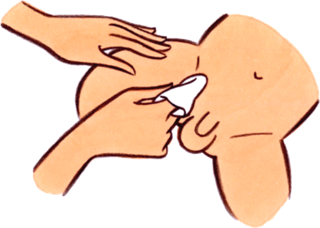
Most intact men discover masturbation by rubbing their foreskin back and forth over the glans, or head of the penis.
Intact male playing with his foreskin
They discover the pleasurable sensations this gives, and eventually find the point of no return learn to go past it. Eventually, they learn to masturbate by grasping the skin on the shaft of the penis and moving the foreskin up and down.
Typical shaft stroke
Shaft hold as seen from the top
Circumcised men learn to masturbate in a similar way, grasping the shaft and moving the hand up and down along it...
...with the exception that most of them find they need the aid of some form of lubricant.
There is an entire market for personal lubricant. Nowadays Albolene and Coconut Oil are very popular.
That is one of the advantages we intact men have; the foreskin provides a natural buffer between our hands an the shaft of the penis, resulting in an ease of masturbation; you're not dependent on a bottle or canister of lube.
The rubbing of the inner mucosa of the foreskin against the mucosa of the glans makes the friction smooth and gentle. Additionally, the foreskin is a double-layered sleeve that rolls over itself, allowing it to glide over the shaft, unlike the skin on the shaft of the circumcised penis, which is immobile. It is a fact that for most intact men, lubrication is not necessary, though some men may choose to use it. It's also not cut-and-dried that circumcised men absolutely need lubrication; some can actually "go dry," though they might find that the friction begins to chafe after a while.
One thing is for sure; having a foreskin makes masturbation easier and more enjoyable. It was making masturbation difficult or impossible for boys and men which attracted early Victorian physicians to the practice of circumcision.
What are other ways in which men masturbate?
Grasping the shaft with the hand and moving it up and down is probably the most common way for men to masturbate, although they have been known to experiment using other methods and techniques.
A different way to masturbate is to reverse one's grip like this:
Some men learn to use a lighter grip, and even develop a technique using only the tips of the fingers, and hold the penis as they would a pen or pencil like this:
Notice the mobility of the skin on the shaft of the penis.
Sometimes men use both hands to rub the shaft between them like this:
Note that having a foreskin makes the above technique easier, as it provides rolling action.
Still more men prefer to use masturbation toys, such as plastic sleeves or tubes, that will allow them to mimic the action of penetrating a vagina. Quite possibly the most famous masturbation toy out there is the Fleshlight, which comes in a variety of styles.
Men can use it to glide up and down the penis...
...or they can fix it in place and thrust into it as they would a partner.
I've only listed some of the more common ways in which men masturbate, but the reality is that there is a whole lot more out there, as different men experiment in different ways.
When I was growing up, one of my go-to resources was a website called JackinWorld.
And recently, as an adult, I found another incredible resource on masturbation called Erotic Engineering. I recommend this website to readers who wish to improve and deepen their masturbation experience.
Masturbation Habits to Avoid
All men, whether they are intact or circumcised, should become aware of a bad masturbation habit known as "death grip."
What Is Death Grip?
The term "death grip" as it pertains to masturbation was originally coined by sex columnist Dan Savage.
The fact is that "death grip" is not something that has been officially recognized, but it describes a condition where men masturbate in a way that is too aggressive, so aggressive that it may be negatively affecting their sex life with their partners, if not affecting the way they enjoy masturbation.
Sex Columnist Dan Savage
The fact is that "death grip" is not something that has been officially recognized, but it describes a condition where men masturbate in a way that is too aggressive, so aggressive that it may be negatively affecting their sex life with their partners, if not affecting the way they enjoy masturbation.
Some men develop a masturbation technique that applies extreme pressure on the penis. They grasp their penis with a tighter and tighter grip, until they get used to extreme sensations, such as the heavy pressure and rough friction that are only possible with a tight grip during masturbation, to the point where actual sex with a partner may be difficult.
Skeptics dismiss "death grip" as a just anorgasmia, but it isn't so simple; men who report using "death grip" to masturbate report that they can still experience pleasure, but that a vagina feels "too loose" and even fellatio does not provide enough pleasure to result in orgasm.
What Causes Death Grip?
It is not known for certain what causes this phenomenon, but people attribute the condition to different causes.
Too Much Porn
It
may be the case that with the free availability of pornography on the
internet, men have become used to extreme, unrealistic fantasies
portrayed in the artificial setting porn, to the point that normal,
real-life average sex isn't so exciting. For this reason, organizations
like NoFap encourage men to abstain from pornography.
Too Much Masturbation
Too Much Masturbation
This looks like it may be linked to pornography, but it isn't always the case; it is possible to masturbate without pornography.
When
men go through puberty and become sexually active (e.g., begin to
masturbate) sex is not usually readily available. A young man will have
learned to masturbate, and masturbate hundreds of times to sexual
fantasies he invents, before finally coming into contact with
pornography and eventually sex with an actual real-life partner happens
for him. He may develop an aggressive masturbatory technique in the
interim that may desensitize him to the sensations of a looser vagina.
Taboo Surrounding Masturbation
Young men learn quickly that speed
and stealth are the name of the game; masturbation is to be conducted in
a quick, hushed manner, always in secret, always hurried so as to not
be discovered by mom, dad or siblings. This being the case, men learn
masturbation techniques for the purpose of ending the masturbation as
quickly and as quiet as possible, not necessarily for the prolonged
enjoyment of pleasurable sensations. Therefore they develop tight grips
and aggressive friction techniques that result in the instant and
intense sensations needed for quick release.
Supine vs Prone Masturbation - My Personal Story
I'm going to come out to you and say that I myself have experienced trouble with orgasm, both during masturbation and with
partnered sexual intercourse. I learned that I was masturbating in a
strange and detrimental way since I was about 16, and I have been
researching the topic of anorgasmia, benign and detrimental masturbation
technique since.
I'd like to begin my story with how I was raised; I grew up in a very conservative, very Christian household where conversations about sex, let alone masturbation, were not allowed. I grew up around a number of male cousins. As children, we would look for opportunities to show each other our penises and what we could do with them. We would find private, secluded places to urinate with each other and show each other our erections. I remember that age 3 or 4, one of my cousins could already fully retract his foreskin to reveal the purple, shiny head of his penis. I remember being transfixed by this act, and I remember feeling like something was wrong with my penis because I couldn't do that, and it hurt to try. Incidentally, my foreskin didn't become retractable until I was 8 or 9.
One day, we were at my aunt's house, in a room, showing each other our penises, when my aunt came in and saw what was happening. She immediately found a belt and started spanking all of us. She told us we were sick and dirty and that we were not to show each other our penises ever again. This alone should sum up to my readers what attitudes concerning sex and masturbation were like in my family. From then on, I learned that there was something wrong with others seeing my penis, and that it had to stay in my pants at all times save for using the bathroom or taking a bath.
I discovered self-pleasure at the age of 8 out on my school playground by complete accident. One day at school, I was playing on one of those huge wooden apparatuses often installed in a large sandbox, complete with monkey bars, bridges, slides and sloping logs.
The bell marking the end of morning recess had rung, and I needed get back down to go and line up with my class. I got onto the nearest log I could, with my penis up against it, and I slid down not even thinking about it. As I slid down, this intense wave of pressure started burning itself from my crotch, slowly engulfing my whole body. The orgasm was so intense I lost consciousness. By the time I woke back up, all the classes had already lined up and gone back into their classrooms. I was embarrassed to arrive at my classroom late; the teacher was asking where I was and she couldn't believe it when I told her that I "fell asleep" at the sandbox.
I'd like to begin my story with how I was raised; I grew up in a very conservative, very Christian household where conversations about sex, let alone masturbation, were not allowed. I grew up around a number of male cousins. As children, we would look for opportunities to show each other our penises and what we could do with them. We would find private, secluded places to urinate with each other and show each other our erections. I remember that age 3 or 4, one of my cousins could already fully retract his foreskin to reveal the purple, shiny head of his penis. I remember being transfixed by this act, and I remember feeling like something was wrong with my penis because I couldn't do that, and it hurt to try. Incidentally, my foreskin didn't become retractable until I was 8 or 9.
One day, we were at my aunt's house, in a room, showing each other our penises, when my aunt came in and saw what was happening. She immediately found a belt and started spanking all of us. She told us we were sick and dirty and that we were not to show each other our penises ever again. This alone should sum up to my readers what attitudes concerning sex and masturbation were like in my family. From then on, I learned that there was something wrong with others seeing my penis, and that it had to stay in my pants at all times save for using the bathroom or taking a bath.
I discovered self-pleasure at the age of 8 out on my school playground by complete accident. One day at school, I was playing on one of those huge wooden apparatuses often installed in a large sandbox, complete with monkey bars, bridges, slides and sloping logs.
It was something like this, but with sand.
The bell marking the end of morning recess had rung, and I needed get back down to go and line up with my class. I got onto the nearest log I could, with my penis up against it, and I slid down not even thinking about it. As I slid down, this intense wave of pressure started burning itself from my crotch, slowly engulfing my whole body. The orgasm was so intense I lost consciousness. By the time I woke back up, all the classes had already lined up and gone back into their classrooms. I was embarrassed to arrive at my classroom late; the teacher was asking where I was and she couldn't believe it when I told her that I "fell asleep" at the sandbox.
From that day on, I was on a
quest to recreate those sensations again. I learned very quickly from
the other teachers that there was something wrong with humping the logs
at school. I had to move operations to underneath the sandbox; I learned
to hump the sand. I couldn't wait until playtime. I could hide under
the wooden apparatus, hump the sand and nobody would know. At home, I
learned I had to hide underneath the bed and hump the carpet, because my
mom told me if I kept humping the couch arms that my guts would spill
out my penis.
Looking back, how I learned to
masturbate resulted in a sort of excommunication from my peers. Words
like "masturbation" and "jacking off" sounded alien to me. At church, I
would often hear sermons about how boys and men shouldn't masturbate. I
used to have this sort of pride in myself because I believed I never
masturbated. Why would I believe I ever did? I never touched myself. I
wasn't a nasty boy like all the others. At school, other boys would ask
me "Do you jack off?" "Jack off?" I'd ask. "Yeah. You know..." and they
would do the classic, familiar motion with a fist.
I didn't know what they were talking about then. I didn't do what they did. I'd say "You're gross. I don't do that." Little did I know...
It wasn't until I was approaching my late teens when I started discovering things on the internet... puberty... circumcision... masturbation... you know, the usual stuff.
I would discover that I was an outlier, and that not only was I always masturbating and just didn't know it, I didn't masturbate in the way most boys and men did. I read on a few websites that men who masturbated by humping pillows and mattresses, otherwise known as the "prone" position, often had trouble when having sexual intercourse with a partner, so I wanted to correct this.
I didn't know what they were talking about then. I didn't do what they did. I'd say "You're gross. I don't do that." Little did I know...
It wasn't until I was approaching my late teens when I started discovering things on the internet... puberty... circumcision... masturbation... you know, the usual stuff.
I would discover that I was an outlier, and that not only was I always masturbating and just didn't know it, I didn't masturbate in the way most boys and men did. I read on a few websites that men who masturbated by humping pillows and mattresses, otherwise known as the "prone" position, often had trouble when having sexual intercourse with a partner, so I wanted to correct this.
Masturbating in the "prone" position
The more I thought about it, the more I wanted to learn to masturbate how other guys did. More and more, I saw the way I masturbated as a disadvantage. The way I masturbated, I could only masturbate if I was in a room with a rug or a carpet; cold tiled floors were a no-go. A bathroom was ideal since I could easily lock the door for privacy, but if there were no rugs, I'd be SOL.
I was a teen through the 90's, a time of desktop computer towers with large heavy screens, separate mice and keyboards hooked up to dial-up America On-Line accounts. If I wanted to masturbate to porn, I needed to bring down the computer screen to my level (down to the floor), or use printed material. That or simply imagine sexy scenes in my head. I had to sign into America On-Line and hope nobody picked up the phone. It was cumbersome to bring down the large heavy CRT monitor, mouse and keyboard every time I wanted to masturbate to porn. It had to be a day when no one was home and I was sure not to be walked on, unless I wanted to explain why the monitor, mouse and keyboard were on the floor.
So having read many websites about this topic, I wanted to start trying to masturbate in the good ol' fashioned way. I remember that taking my hand and moving my fist up and down did almost nothing for me. I tried many times, but I would always revert to humping the carpet. I would do this completely flaccid and with pants on, by the way. The way I masturbated, I had to learn to wait until my erection died down, and I could position my crotch with my flaccid penis up against the carpet to hump up and down. After many attempts to masturbate my erect member with my hand, I came to the realization that I couldn't masturbate like most guys did. It made me feel like a freak. It felt almost like when I didn't know how to ride a bike or whistle.
Then
I read on a website, I can't remember which one, that it's possible to
learn to masturbate sitting face up with the hand, otherwise known as
the "supine position" if one abstained for a few days before trying. No
touching the penis, no looking at porn, nothing. And then, after a
while, sit down and learn to appreciate subtle sensations. So I decided
to try doing that.
How most men masturbate: "supine" position
College was approaching, and I decided I didn't want to start life as a college student with that problem, so I made it a point to abstain for like 15 days and learn to masturbate "the right way" once and for all. During my first month as a freshman, I decided to have a masturbation session while my roommate was away. I started touching myself, and I started imagining sexy thoughts. I remember it took a while, and I remember it was the strangest sensation to approach orgasm with my hard penis in my hand. I was used to orgasming and ejaculating while humping the floor, completely soft, but this was different. I remember it taking a long time because I just wasn't used to it.
After a long, long time, and me vigorously pumping away, I finally allowed myself to cum. I had no idea how I'd handle it. Being intact, I would always cum in my foreskin. My pants were up the whole time (it's not necessary to undress when humping the floor, making it all that much more convenient), so I didn't have to deal with a mess. I'd just go to the bathroom afterwards, stand over the toilet, unzip, pull my foreskin back and let all the cum drip into the bowl. This time, I had cum all over my hands and clothes. It was the first time in my life that I ever ejaculated while having an erection. I remember it was exciting for me because up until that point, I had never witnessed my penis shoot sperm with my own eyes.
But that excitement was to be short lived, because I heard my roommate put the key in the knob to unlock it, and I had to pull my covers over me and pretend I was asleep until he left. I think he might have been able to tell that the room smelt of cum.
I experienced a mixture of feelings; excitement at finally having been able to masturbate with my hand, relief at finally achieving my goal, embarrassment at almost being "caught," grossness and helplessness at remembering I had no choice but to pull my covers over and onto my cum-covered body, and a bit of anger at my roommate for coming back earlier than expected, even though this was completely my fault and should have made sure he wasn't coming back soon. But all in all, I felt relieved that I was finally able to masturbate the way most other guys did.
That night, I had a huge load (pun absolutely intended)
of laundry to do.
The story doesn't end there, though.
The story doesn't end there, though.
I
had learned to masturbate with my hand, but it still took forever, as I
still wasn't used to masturbating this way. So while I could cum on a
dime when it came to humping the floor, it took me ages to reach orgasm
using my hand. It took forever, and I was squeezing so hard my penis
hurt after masturbation every time. I had weaned myself off of humping
the floor, but now I had, what I now know as "death grip."
Fast-forward to when I started having sex with partners, and the problem reared its ugly head; while it felt fulfilling to have sex with my female partners, it was simply fact that I did "take forever," as it were. The best sensations, at the time, were of me humping the floor, better than even "death grip" masturbation. I had to do something.
How do experts recommend getting rid of Death Grip?
Having read different resources on this topic, I noticed that there are some suggestions by experts that keep recurring.
The first thing many experts recommend is making it a point to change ones' masturbation habits. This should be easy enough, but from the experience of someone who has struggled through this, it's easier said than done. It requires making a conscious effort and patience. Becoming frustrated with not seeing immediate results, it's always easy to revert to old habits to achieve that gratification one already knows how to get so easily, so it's important to resolve to make it a point to make a change, and to keep toward that goal.
The second thing many experts recommend is a long, sustained period of abstinence before attempting to start changing one's masturbation habits. During this abstinence period, a man shouldn't look at porn, or even touch himself in a sexual way. The idea is that a man has become accustomed to intense visual and physical stimuli (e.g. extreme sexual fantasies that only exist in porn, and the extremely high pressure of a tightly clenched fist on the penis), and so his thresholds of stimuli must be "reset."
NoFap calls this "rebooting the brain to factory settings."
Finally, experts recommend, having gone through that period of abstinence, to actually learn healthy masturbation habits. From this moment on, a man has to make it a point to masturbate and achieve orgasm only in the supine position, if he used to masturbate prone. Instead of a tight grip, a man should masturbate learning to listen to and enjoy the subtle sensations of light touch. Men are encouraged to use lubrication and a lighter grip that more closely resembles the soft tissues of the vagina. Some websites recommend using a penetrative sex toy that allows a man to mimic vaginal sex, such as a Fleshlight.
Still other experts recommend men learn to masturbate in the absence of porn. Instead, of masturbating while watching porn, they recommend watching it, but then turning it off and masturbate using only the imagination.
"Don't touch yourself while you watch porn. Soak up the images, saver it and get crazy turned on. Then, turn off the laptop, go to another room and replay the images in your mind while you masturbate. This allows you to tune more into the sensations in your penis, without the distraction from all the input to your eyes," says certified sex coach Sarah Martin, MA.
I think this is an important point, because a dependency on pornography limits a man in the sense that, he can only ever masturbate if he has a laptop or porn mags. I myself don't think there's anything wrong with pornography, but I don't want to have to depend on it to get off.
All experts agree that teaching the body to enjoy new and less intense stimulation will take time and patience. If you feel yourself reverting to old habits, you have to learn to have the will power to stop and not allow yourself to go back.
The Conclusion to My Story
I was eventually able to wean myself off of using the floor to masturbate, but I still had this lingering problem of not having full control of my orgasms. From time to time, I still found myself resorting to "death grip." It's embarrassing to admit, but sometimes I took forever to orgasm with my wife. Fellatio felt OK, but never satisfying enough to bring me off to orgasm. On more than one occasion we had to stop because it wasn't going anywhere. It was embarrassing to just say "Let's call it a day," and then go off and hide somewhere and finish off my hand.
It was clear; it wasn't a problem with ED or anorgasmia. I could demontrably get an erection, and I could ejaculate if I masturbated aggressively to porn, and I know for a fact if I humped the floor, I could cum in under 30 seconds.
The problem was that I had become used to masturbating only to porn, and masturbating only with heavy pressure on my poor dick.
I sought to find a way to "cure" myself of this.
I wanted so bad to gain control of my orgasm, and to be able to enjoy sex and masturbation like any other guy would.
I had heard of NoFap and No Nut November, and I already knew that at some point or another, I needed to commit myself to a "reboot" period if I was serious about relearning how to masturbate.
So last year, last November, I told myself "this is it." I decided that for at least once in my life, I was going to abstain for 30 days, and that it was going to be November of 2018.
What could it hurt?
For 30 days, I abstained from any sexual activity; no masturbation, no touching myself, nothing.
By the end, after 30 days of fighting back the urge to masturbate, I was curious about what masturbation was going to feel like. Marked on my calendar was the night of the 30th when I would break my masturbation fast. "Bate-fast" I'd like to call it.
I swear I had never felt my erection so huge in my hands, and I had never been so sensitive. I wasn't gripping, I wasn't rushing, and I felt I had full control of when I was about to orgasm.
Call it the feeling of success, call it "just relief after 30 days," but I must say that after 30 days of absolutely no sexual activity, I had the most sensational masturbation session, possibly the best ever in my whole life.
For the first time in my life I experienced something different; perhaps it was due to the fact that I had 30 days' worth of cum in me, but I noticed that after I ejaculated initially, I somehow felt as if the orgasm was ongoing. Involuntarily, my penis ejaculated a 2nd time. Like within seconds of my first ejaculation.
I was like "Woah shit!!! That's never happened before!!!"
Fast-forward to when I started having sex with partners, and the problem reared its ugly head; while it felt fulfilling to have sex with my female partners, it was simply fact that I did "take forever," as it were. The best sensations, at the time, were of me humping the floor, better than even "death grip" masturbation. I had to do something.
How do experts recommend getting rid of Death Grip?
Having read different resources on this topic, I noticed that there are some suggestions by experts that keep recurring.
The first thing many experts recommend is making it a point to change ones' masturbation habits. This should be easy enough, but from the experience of someone who has struggled through this, it's easier said than done. It requires making a conscious effort and patience. Becoming frustrated with not seeing immediate results, it's always easy to revert to old habits to achieve that gratification one already knows how to get so easily, so it's important to resolve to make it a point to make a change, and to keep toward that goal.
The second thing many experts recommend is a long, sustained period of abstinence before attempting to start changing one's masturbation habits. During this abstinence period, a man shouldn't look at porn, or even touch himself in a sexual way. The idea is that a man has become accustomed to intense visual and physical stimuli (e.g. extreme sexual fantasies that only exist in porn, and the extremely high pressure of a tightly clenched fist on the penis), and so his thresholds of stimuli must be "reset."
NoFap calls this "rebooting the brain to factory settings."
Finally, experts recommend, having gone through that period of abstinence, to actually learn healthy masturbation habits. From this moment on, a man has to make it a point to masturbate and achieve orgasm only in the supine position, if he used to masturbate prone. Instead of a tight grip, a man should masturbate learning to listen to and enjoy the subtle sensations of light touch. Men are encouraged to use lubrication and a lighter grip that more closely resembles the soft tissues of the vagina. Some websites recommend using a penetrative sex toy that allows a man to mimic vaginal sex, such as a Fleshlight.
Still other experts recommend men learn to masturbate in the absence of porn. Instead, of masturbating while watching porn, they recommend watching it, but then turning it off and masturbate using only the imagination.
"Don't touch yourself while you watch porn. Soak up the images, saver it and get crazy turned on. Then, turn off the laptop, go to another room and replay the images in your mind while you masturbate. This allows you to tune more into the sensations in your penis, without the distraction from all the input to your eyes," says certified sex coach Sarah Martin, MA.
I think this is an important point, because a dependency on pornography limits a man in the sense that, he can only ever masturbate if he has a laptop or porn mags. I myself don't think there's anything wrong with pornography, but I don't want to have to depend on it to get off.
All experts agree that teaching the body to enjoy new and less intense stimulation will take time and patience. If you feel yourself reverting to old habits, you have to learn to have the will power to stop and not allow yourself to go back.
The Conclusion to My Story
I was eventually able to wean myself off of using the floor to masturbate, but I still had this lingering problem of not having full control of my orgasms. From time to time, I still found myself resorting to "death grip." It's embarrassing to admit, but sometimes I took forever to orgasm with my wife. Fellatio felt OK, but never satisfying enough to bring me off to orgasm. On more than one occasion we had to stop because it wasn't going anywhere. It was embarrassing to just say "Let's call it a day," and then go off and hide somewhere and finish off my hand.
It was clear; it wasn't a problem with ED or anorgasmia. I could demontrably get an erection, and I could ejaculate if I masturbated aggressively to porn, and I know for a fact if I humped the floor, I could cum in under 30 seconds.
The problem was that I had become used to masturbating only to porn, and masturbating only with heavy pressure on my poor dick.
I sought to find a way to "cure" myself of this.
I wanted so bad to gain control of my orgasm, and to be able to enjoy sex and masturbation like any other guy would.
I had heard of NoFap and No Nut November, and I already knew that at some point or another, I needed to commit myself to a "reboot" period if I was serious about relearning how to masturbate.
So last year, last November, I told myself "this is it." I decided that for at least once in my life, I was going to abstain for 30 days, and that it was going to be November of 2018.
What could it hurt?
For 30 days, I abstained from any sexual activity; no masturbation, no touching myself, nothing.
By the end, after 30 days of fighting back the urge to masturbate, I was curious about what masturbation was going to feel like. Marked on my calendar was the night of the 30th when I would break my masturbation fast. "Bate-fast" I'd like to call it.
I swear I had never felt my erection so huge in my hands, and I had never been so sensitive. I wasn't gripping, I wasn't rushing, and I felt I had full control of when I was about to orgasm.
Call it the feeling of success, call it "just relief after 30 days," but I must say that after 30 days of absolutely no sexual activity, I had the most sensational masturbation session, possibly the best ever in my whole life.
For the first time in my life I experienced something different; perhaps it was due to the fact that I had 30 days' worth of cum in me, but I noticed that after I ejaculated initially, I somehow felt as if the orgasm was ongoing. Involuntarily, my penis ejaculated a 2nd time. Like within seconds of my first ejaculation.
I was like "Woah shit!!! That's never happened before!!!"
Not only was my masturbation experience better than ever, this also translated to better sex with my wife. For the first time in my life I felt like I could go as long or as short as we wanted. I became convinced that abstaining from masturbation can actually be a good thing.
The
moral of the story is that how a man learns to masturbate could
influence whether or not he develops detrimental self-pleasure
techniques, and ultimately, how he has sex with a partner.
I think that if men would be allowed to discuss masturbation openly with one another, the world would be a better place. If men discussed how they masturbated, and maybe even mentored each other on benign and detrimental ways of masturbating, perhaps they would learn how to avoid problems such as "death grip" and improve their solo, as well as partnered sex lives.
I admit this could sound creepy to some, but in retrospect, I really wish someone would have talked to me about masturbation. I wish somebody would have told me "You're doing it wrong. You should try masturbating how most men do it." I think it would have saved me lots of trouble.
I think that if men would be allowed to discuss masturbation openly with one another, the world would be a better place. If men discussed how they masturbated, and maybe even mentored each other on benign and detrimental ways of masturbating, perhaps they would learn how to avoid problems such as "death grip" and improve their solo, as well as partnered sex lives.
I admit this could sound creepy to some, but in retrospect, I really wish someone would have talked to me about masturbation. I wish somebody would have told me "You're doing it wrong. You should try masturbating how most men do it." I think it would have saved me lots of trouble.
Circumcised vs Intact
There
is still one more elephant-in-the-room factor that I believe may
contribute to the development of "death grip" and that is circumcision
status.
It had been long known since the time of John Harvey Kellogg that circumcision made masturbation difficult. It was known for longer than that, as Rabbi Maimonides wrote in his book "A Guide for the Perplexed" that circumcision was supposed to render the male organ to make it "as quiet as possible."
It had been long known since the time of John Harvey Kellogg that circumcision made masturbation difficult. It was known for longer than that, as Rabbi Maimonides wrote in his book "A Guide for the Perplexed" that circumcision was supposed to render the male organ to make it "as quiet as possible."
Moses "Rambam" Maimonides (1135-1204)
"...with regard to circumcision, one of the reasons for it is, in my opinion, the wish to bring about a decrease in sexual intercourse and a weakening of the organ in question, so that this activity be diminished and the organ be in as quiet a state as possible"~"A Guide for the Perplexed" Part III, Chapter 49, Page 609Circumcision may contribute to a desensitization of the penis, because it removes the most sensitive part of the penis. Sorrells et al. measured sensitivity along different points of the penis in intact and circumcised men, and found published their findings in the British Journal of Urology.
Findings by Sorrells et al.: Circumcision removes the most sensitive part of the penis.
On their Death Grip article, Men's Health says "There may be a link to masturbation with death grip and penile nerve damage, but there currently isn't enough scientific data to support this conclusion."
This is an interesting passage, because it is simply irrefutable fact that circumcision is deliberate nerve damage; it is the cutting away of the most sensitive of nerves on the penis. In addition to removing sensitive areas on the penis, the lack of a foreskin causes the mucosal tissue of the glans and remaining inner part of the foreskin to become dried out and hardened in a process called "keratinization," which could result in further desensitizing the penis.
The glans in intact and circumcised penes
With all this nerve removal and keritinization, could it be that men are developing aggressive masturbation techniques as a result of being circumcised?
Could there a correlation?
I
don't know. As I've already let readers know, I experienced this
phenomenon of "death grip" and a difficult time reaching orgasm by
manual masturbation and with a partner, even though I'm not circumcised,
so it may be possible that both intact and circumcised men may be
susceptible to this phenomenon, albeit to different degrees.
The world may never know until scientists decide to break with taboo and actually investigate this. It's nearly 2020 and people STILL have hangups about sex and masturbation.
Results on a quick Twitter Poll
It may not amount to much, if anything this could be a good start for other interested researchers to follow, but for now, I have conducted a quick Twitter poll asking for men to self-report whether or not they are struggling with "death grip" and their circumcision status, and here are the results:
The world may never know until scientists decide to break with taboo and actually investigate this. It's nearly 2020 and people STILL have hangups about sex and masturbation.
Results on a quick Twitter Poll
It may not amount to much, if anything this could be a good start for other interested researchers to follow, but for now, I have conducted a quick Twitter poll asking for men to self-report whether or not they are struggling with "death grip" and their circumcision status, and here are the results:
Up front, it must be said that 40 respondents isn't a huge sample size, but I'm still posting these results for what it's worth.
Here are my observations:
There were slightly more circumcised respondents than intact.
On either side, there were more respondents that reported they weren't experiencing "death grip," as opposed to those who reported they were.
I want to bring attention to the difference in intact and circumcised men who reported they were experiencing "death grip"; there were far more circumcised men than intact men.
The greater number of respondents were intact men reporting they were not experiencing "death grip."
Is there a correlation between circumcision and a higher rate of men experiencing "death grip?"
Again, this isn't definitive by any means, as the sample size is rather small, but if these numbers mean anything, it seems more circumcised men may be experiencing the phenomenon of "death grip" than intact men.
This was an informal poll with a very small sample size, but I hope this might serve as a starting point for others interested in exploring this further.
That's all she wrote for today!
External Links:#NoNutNovember Poll— Joseph Lewis (@Joseph4GI) November 12, 2019
Do you have #deathgrip?
What’s your circumcision status?
Be honest! 😏#nofap #nofapnovember
Men's Health Death Grip Article
Death Grip Article on Vice
"How to cure death grip"